See also: Diabetes Complications: Heart, Kidney, Eye, and Foot Health — our complete pillar guide.
If high blood sugar is the kindling, high blood pressure is the gasoline that fuels the fire of diabetic kidney disease. Controlling blood pressure is just as important as controlling blood sugar for preserving kidney function. But what should the target be?
The Evolving Guidelines
For a long time, the standard blood pressure target for people with diabetes was less than 140/90 mmHg. However, as research has evolved, guidelines have become more stringent, especially for individuals with signs of kidney disease.
Current recommendations from organizations like the American Diabetes Association (ADA) and KDIGO (Kidney Disease: Improving Global Outcomes) suggest a target of **less than 130/80 mmHg** for most people with diabetes and hypertension. For those who already have chronic kidney disease (CKD), some experts advocate for even tighter control, aiming for a systolic pressure (the top number) closer to 120 mmHg, if it can be achieved safely without causing side effects like dizziness.
Why Tighter Control? Every point you lower your blood pressure reduces the strain on the delicate blood vessels in your kidneys. Think of it like a plumbing system: lower pressure means less wear and tear on the pipes. This slows down the process of damage and scarring.
Medications: Not Just for Blood Pressure
For people with diabetes and high blood pressure, the choice of medication is key. Two classes of drugs are considered first-line therapy because they provide direct kidney protection in addition to lowering blood pressure:
- ACE (Angiotensin-Converting Enzyme) Inhibitors: Drugs ending in “-pril” (e.g., lisinopril, ramipril).
- ARBs (Angiotensin II Receptor Blockers): Drugs ending in “-sartan” (e.g., losartan, valsartan).
These medications work by relaxing blood vessels, but they also have a specific beneficial effect on the pressure within the glomeruli, the kidney’s filters. They are a cornerstone of therapy for anyone with diabetes and albuminuria (protein in the urine), even if their blood pressure is not yet considered high.
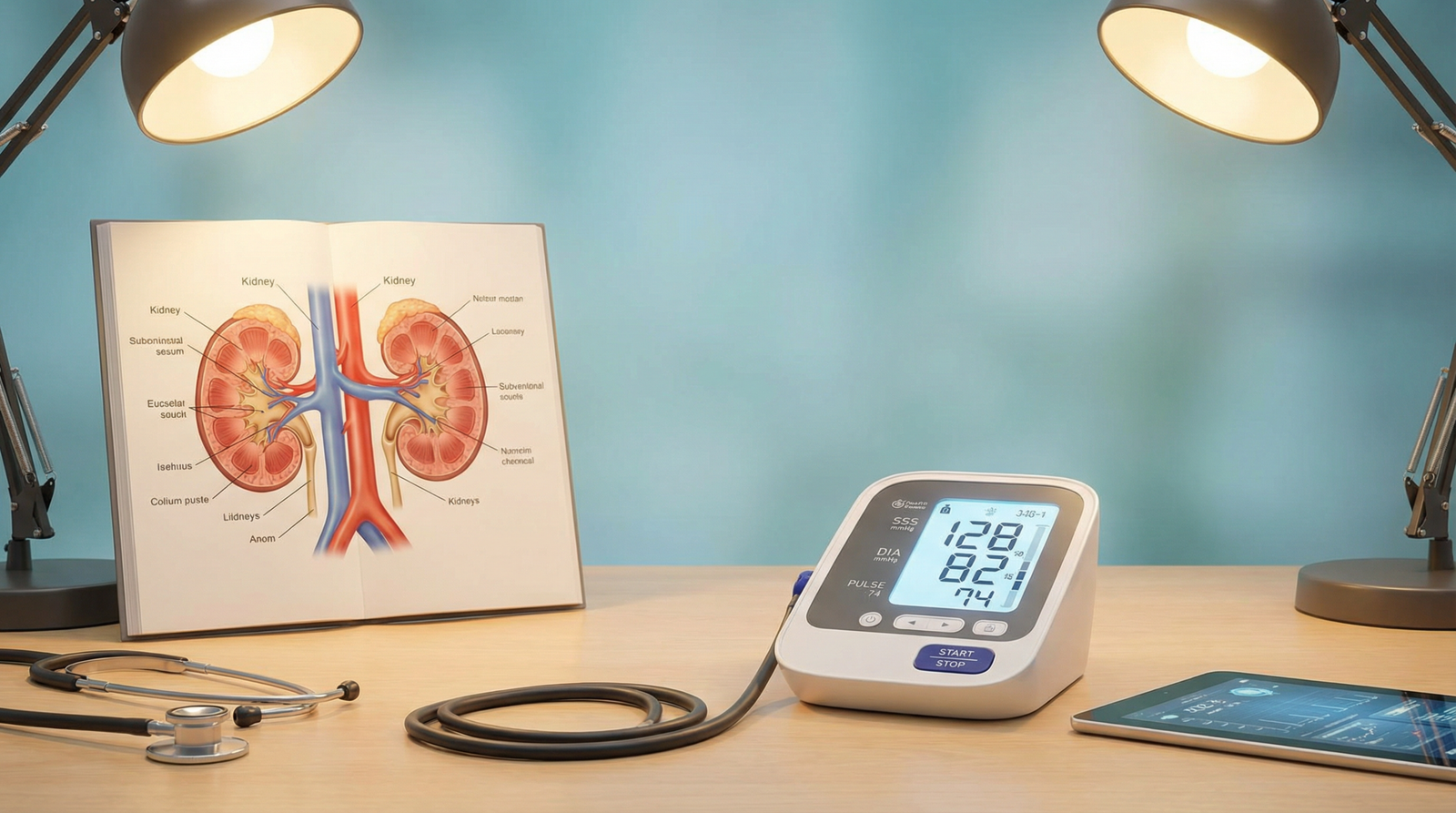
The Importance of Home Monitoring
Your blood pressure can vary throughout the day and can be artificially high in a doctor’s office (a phenomenon known as “white coat hypertension”). Regularly monitoring your blood pressure at home provides a much more accurate picture of your true average blood pressure. Share your home readings with your doctor to help them make the best treatment decisions.
Key Takeaway
For optimal kidney protection, aim for a blood pressure target of less than 130/80 mmHg, and possibly even lower if you have existing CKD. Medications like ACE inhibitors and ARBs are essential tools, and regular home monitoring is crucial for effective management. Don’t underestimate the power of blood pressure control in your fight to preserve kidney health.